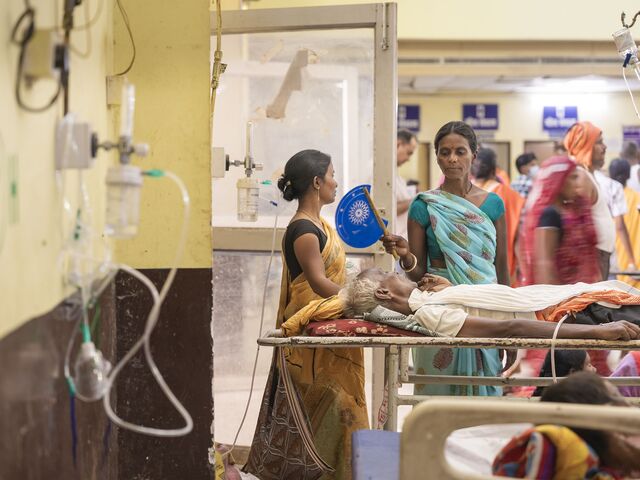
India’s Boiling Point
Millions in the country are confronting a terrifying reality: When sweat can’t evaporate, heat kills.
When Gyanchand Saw climbed out of his car on a sweltering morning in mid-May, his son, sitting in the driver’s seat, noticed beads of sweat trickling down the 55-year-old’s forehead. Saw greeted a friend, exchanged a few words, then began to struggle. His body crumpled, and he fell to the ground.
Panicked, Saw’s son carried him back into the vehicle and began weaving through the traffic-clogged center of Gaya, a small city in eastern India, trying to find help. The family eventually brought him to the Anugrah Narayan Magadh Medical College & Hospital (ANMMCH), where the waiting area was already crowded with other patients and their families. On a stretcher, Saw lay still. A doctor ran over with a technician close behind, wheeling an electrocardiogram machine. After checking Saw’s pulse, they connected the wires of the device to his chest and then watched as it printed the result on a roll of white paper: an unforgiving straight line.
Breaking down in sobs around his body, Saw’s kin tried to make sense of what had just occurred. A building contractor by trade, Saw had been on medication for a heart problem but was otherwise healthy, robust enough to spend his days working outdoors and traveling between jobs by motorcycle in all kinds of weather. Hospital staff said they couldn’t provide a definitive cause of death until they’d conducted a postmortem. Sanjay Suman, the friend Saw was with when he collapsed, had no doubt what had happened: “From the moment he stepped out of the car,” Suman said, “he was complaining about the heat. If it were not for this heat, he would still be here.”
As climate change transforms life in India, and much of the developing world, stories like Saw’s are becoming more and more common. Ten out of the country’s 15 hottest years on record were in the last decade and a half; in 2024, New Delhi experienced daytime temperatures higher than 40C (104F) for an entire month. With humidity, the air can feel as much as 10 degrees hotter. Even in a nation that’s made huge strides in modernizing its economy, such temperatures can overwhelm railways and electrical grids, hampering exports and idling factories.
They can also cause severe illness or death. And for hundreds of millions of Indians, the best option for help is to travel to somewhere like the ANMMCH. To understand the scale of the challenge, reporters for Bloomberg Businessweek made five visits to the government-run facility during the hottest time of the year: April, May and early June, before the monsoon rains bring relief. In many ways the low-rise building, which dates to the 1960s, is typical of medical centers across the country. Its wards are packed day and night with patients and their relatives, some of whom have traveled for hours in buses and rickshaws. The emergency room has no air conditioning, and its high, cobweb-covered windows are sealed, with the only cooling coming from slow-moving fans.

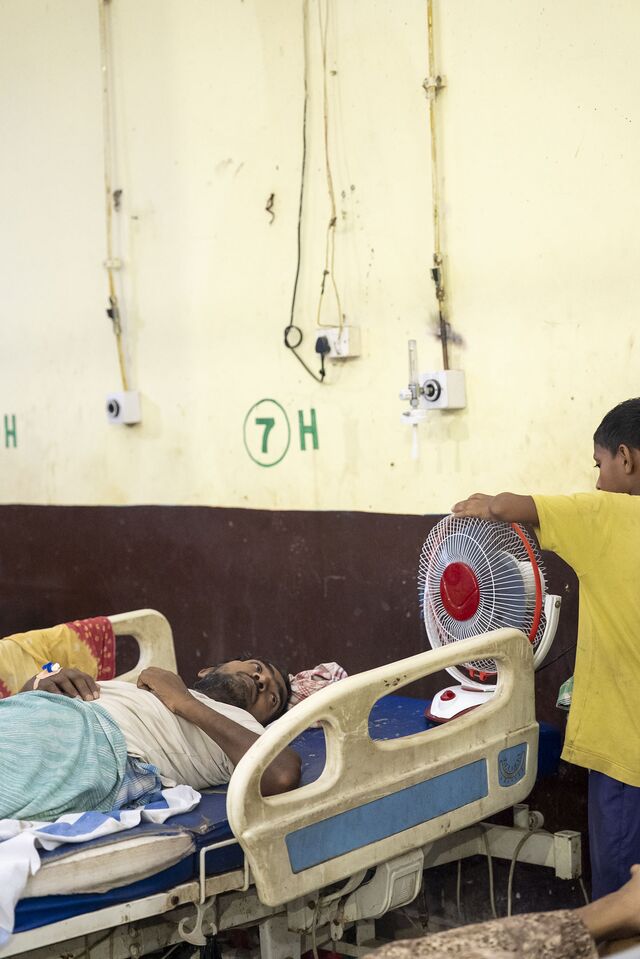
The most recent hot season was relatively moderate, with the daytime mercury in Gaya hovering around 35C, compared with a record-breaking 47C in 2024. The reporters nonetheless watched doctors and nurses treat a constant stream of patients for heat-linked ailments, from dehydration to heart complaints to breathing problems—a flow that intensified or slackened with the temperature. Inside it was only a few degrees cooler than on the street, and by midafternoon, moving around was physically taxing. Patients sat drenched in sweat, waiting to be seen by one of the two dozen medical staff working in the ER. With few chairs, many sat on the floor or on stretchers, their saline drips hung on nails or held aloft by family members.
The toll of what researchers call “heat stress” is growing rapidly in India. Almost three-quarters of the workforce labors either outside or in indoor settings that have little to no cooling. Many are employed informally, and, in addition to the consequences for their health, those who collapse from heatstroke or dehydration forgo the income they need to survive. They also can’t contribute to the growth of the economy. According to the International Labour Organization, heat stress will reduce India’s annual productivity by the equivalent of 34 million full-time jobs by the end of the decade; the McKinsey Global Institute estimates that as much as 4.5% of the country’s gross domestic product, or roughly $250 billion, could be at risk from such lost work.
High Heat Risk Covers India, and Humidity Is Making It Worse
Although Prime Minister Narendra Modi’s government has acknowledged that India needs a better strategy for dealing with heat, its concrete responses have so far been modest. There’s no comprehensive national system for tracking deaths from heat, and only limited funds are available for long-term adaptation efforts, such as mapping urban areas that are at risk or planting trees to cool down those scorching cities.
That leaves medical professionals in places such as ANMMCH working furiously to help their patients—overwhelmingly, laborers who don’t have the luxury of taking time off when the temperature is dangerously high. If they stay outside long enough, they can find their brain function disrupted, causing dizziness and confusion. Internal organs can be deprived of blood and oxygen. Without prompt treatment, damage can be permanent. “There’s not one system in the body that heat spares,” says Kamlesh Kumar, the director of ANMMCH’s heat-response department. “Right from the central nervous system—to our heart, to our muscles, kidneys and liver—everything is at risk.”
In the opening scenes of The Ministry for the Future, Kim Stanley Robinson’s dystopian novel, India is hit with the most severe heat wave in its history. The electric grid fails, taps run dry, and criminal gangs hunt for air conditioners. A desperate crowd seeks refuge in a lake, where the water proves fatally hot. Across the country, 20 million people die.
Robinson’s fictional scenario was built on a real scientific principle. When the air is both hot and humid enough, sweat can’t evaporate, and therefore the body can’t cool. This risk is measured by what’s called a wet-bulb temperature—essentially the reading on a thermometer that’s been wrapped in a wet cloth. Sustained exposure to a WBT higher than 30C is risky for humans; above 35C it’s almost certainly fatal.
The US and Europe rarely see such highs, even in their hottest periods. During New York’s June heat wave, the WBT generally remained below 30C. India, with its hot-season combination of extreme temperatures and humidity, is different. According to one study, about 70% of Indians could be exposed to a WBT of 32C or more by the end of this century. In that scenario, about 2% of the population—tens of millions of people—could be beyond the 35C threshold. Long before reaching those levels, agriculture would grind almost to a halt in the affected regions, threatening the food supply.


Bihar, the state that includes Gaya, is both hot and populous even by Indian standards; its 130 million people regularly experience a WBT above 30C. Add in pollution from cars, trucks and motorbikes, and even the simple act of breathing can be difficult. The effects are especially problematic in fast-growing provincial cities, with their dusty streets and almost nonexistent green spaces. Children and the elderly struggle first, but healthy adults soon follow.
The dangers of extreme heat have become tragically apparent in the state over the past decade. A 2019 heat wave killed at least 215 people in Bihar, and during last year’s national election, 10 poll workers died of apparent heatstroke within 24 hours, according to Indian media reports. Such figures are almost certainly dramatic underestimates. In many cases heat aggravates preexisting medical conditions, which then get listed as the cause of death. Meanwhile, Bihar has one of the lowest death registration rates in the country—some estimates suggest at least a third of fatalities from all causes are never recorded in any official database.
Much of India’s planning for heat stress focuses on such extreme conditions, which obviously represent emergencies. But some experts worry that focusing on them risks obscuring another problem. “We think about preparing for disaster, when thresholds are crossed. But what about a prolonged, chronic heat event?” asks Ronita Bardhan, an architectural engineer and a professor at the University of Cambridge who studies the impact of heat. A “zone of distress” sits just below the hottest temperatures, she adds, and it can still result in grave problems for people and infrastructure: “With hotter summers, India will come up against this more often.”
Bihar does have a heat-action plan, produced in 2019. It includes deploying alert systems for imminent hot weather, proposals to educate citizens about its dangers and blueprints for expanded medical support. But the state government hasn’t allocated any dedicated funding, and many of the plan’s recommendations have yet to be implemented. Only a handful of people interviewed during Businessweek’s visits to ANMMCH were even aware of official warnings. When the heat reaches life-threatening levels, people in cities like Gaya are mostly on their own—unless they can get to a hospital.

In the emergency room, Shanti Devi lay almost motionless on a thin mattress, taking shallow breaths through her oxygen mask. She wore a faded yellow and red sari, draped loosely over her gaunt body. Even at 72, she’d normally be working in the fields with her family, earning about 300 rupees ($3.43) a day alongside her son, daughter and daughter-in-law. Devi was sowing the monsoon crop when she fell ill two weeks earlier and developed a severe fever.
After her condition deteriorated further, her family spent more than 10 times her daily wage on a taxi to ANMMCH. Then they waited much of the day for her to be seen, worrying that the expense had been in vain. Eventually nurses began some tests; it took them three attempts to draw Devi’s blood. Soon they started planning to move her into an inpatient ward. Keeping her in hospital and away from work would cost her family dearly, in direct expenses and forgone wages, but after coming this far, they felt they had no option but to wait for treatment. “She works too hard. She’s ill because of heat and exhaustion,” said Ranti Kumari, her daughter. Alongside her, Devi’s daughter-in-law said she’d received no alerts from the government about heat risks, nor any information on what to do about them. “We are poor people who work as laborers,” Kumari explained. “We don’t have smartphones or televisions to know about heat.”
Devi and patients like her are ultimately the responsibility of Kamlesh Kumar, who, in addition to leading the hospital’s heat response, is one of its senior-most general physicians. On a cooler day, Businessweek reporters found him doing rounds on the third floor, checking on a frail man with a swollen abdomen, an elderly woman struggling with breathlessness and a young girl recovering from viral meningitis.
As he walked the corridors with medical students, Kumar lobbed good-natured questions, quizzing them on symptoms and conditions. At the end of one room, he asked nurses about the test results for a 25-year-old man who sat staring silently at the windows in front of him. Kumar placed a gloved hand on his shoulder and asked how he felt; the patient began to weep. Before being admitted, he’d attempted suicide, staff confided later.
Back in his cramped office, Kumar said that in hotter weather he wouldn’t be able to devote this kind of time to regular cases: “If there’s a sudden influx of heatstroke patients, you wouldn’t find me here.” Such a surge could push the hospital well past its limits. On average the ER receives about 200 patients a day—four times the number doctors said they could comfortably handle.
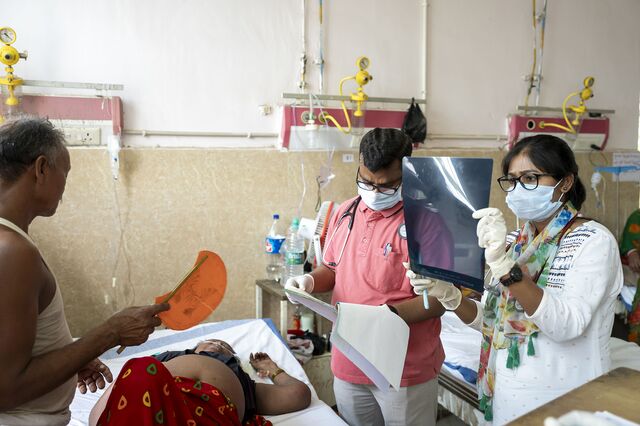
The same morning’s queue included a young girl whose panic attacks had prompted a doctor to prescribe an EKG, but only when she could find a place to lie down. With no beds or stretchers available, her family eventually pulled together three chairs. Meanwhile a man with a bandaged head moved around carrying his own bottle of IV fluid. Another was forced by the lack of wheelchairs to transport his elderly father on his shoulders as a doctor measured the father’s oxygen saturation. Patients waited for hours in halls filled with family members and a powerful smell of disinfectant and sweat.
Yet, remarkably, the best-equipped part of ANMMCH sat empty: the dedicated heat ward. Built with repurposed Covid-19 funds, the 96-bed wing is pristine, with clean blue curtains, spotless floors and air conditioners whirring overhead. Workers keep diesel generators on standby, ready to run the cooling systems in case of a power failure. Leaving it idle might seem illogical, but Kumar and his colleagues explained their reasoning. When the worst heat strikes, patient numbers can spike with astonishing speed; of the hospital’s 201 cases of heatstroke in 2024, about a quarter arrived on a single day. Ten heatstroke patients, all with serious preexisting conditions, ultimately died.
The ward is therefore reserved for use only during heat waves, typically when temperatures exceed 42C. Until then, doctors and nurses make do with their usual, run-down facilities. It’s an example, in microcosm, of the dilemma identified by Cambridge’s Bardhan: Focusing on the worst emergencies may leave India underprepared for the slower-moving crisis playing out in its cities every summer.



Officials at all levels of government in India acknowledge they need to do more to manage the impact of heat. In Bihar the authorities say they’re planning to hire more doctors and, in the medium term, open more large hospitals like ANMMCH. The state is also attempting to improve the quality of small clinics, which have long had a reputation for patchy care. In 2005 the average local clinic received just 39 patients a month, says Manoj Kumar Singh, who served until recently as the No. 2 bureaucrat in the Bihar health department. Today that number is 11,000, growth he attributes to recent investments in staffing and supplies. “Clearly their faith in primary health-care centers has improved,” Singh says. “We have built up capacities. I’m not saying we’re perfect, far from it, but things have improved tremendously.”
To critics, however, the government’s efforts are too reactive, focused on mitigating the worst medical consequences of heat, rather than on more fundamental changes: for example, overhauling the infrastructure of India’s cities to make them cooler, with shade and green spaces. Nor has the Modi government been willing, so far, to take a stronger position on climate change. India is the world’s third-largest carbon emitter, behind China and the US, and a major user of coal power, which successive governments have said is essential to providing its vast population with energy. “We need structural fixes,” says Aditya Valiathan Pillai, a visiting fellow at the Sustainable Futures Collaborative in New Delhi who researches climate adaptation. “We really need to build a country that is capable of dealing with a changing climate.”

In the ANMMCH emergency room, that can feel like a distant prospect. On a late April day, with temperatures that peaked at 36C amid intense humidity, the hospital’s corridors were stifling. One of the patients waiting to be seen was Prakash Manjhi, a 14-year-old who began to feel ill after playing in the afternoon sun. He soon had a fever and started to vomit—common symptoms of heatstroke.
Manjhi’s parents eventually decided to bring him to Gaya, 50 kilometers (31 miles) from their home village. It was a major decision for the family, which gets by on about 10,000 rupees a month; his father, Sudhir, had to borrow money from relatives to pay for the journey. Treatment in Gaya was free, but other costs were mounting. To help care for his son, Sudhir had been away from his job as a farm laborer for almost eight days, a break he could hardly afford.
One option would be for his wife to start working when they returned home, helping to close the financial gap. But Sudhir was skeptical that would make any difference to the family’s situation. “What’s the point?” he asked. “She will work in extreme heat, and if she falls ill, we’ll end up spending more than we can earn.”
